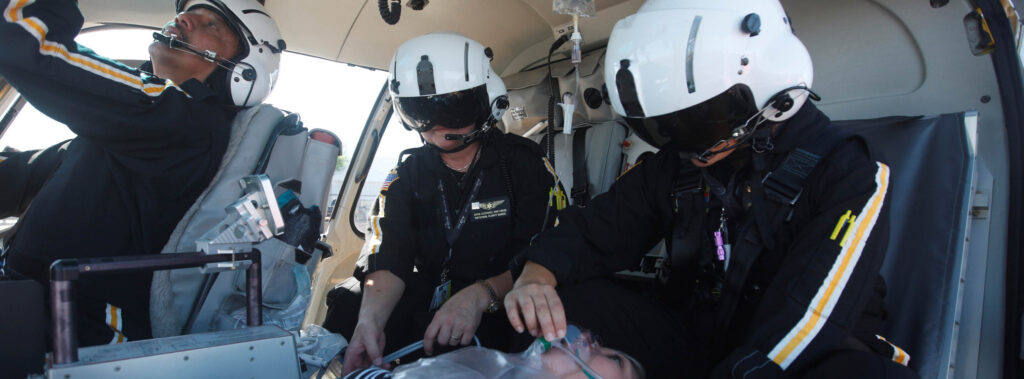
High-Risk Pregnancy Air Transport: How PHI Air Medical and PHI Cares Protect Families
When a high-risk pregnancy complication strikes in a rural community, minutes matter. Severe preeclampsia, placental abruption, premature labor, and postpartum hemorrhage can all escalate quickly — and the nearest hospital often cannot provide the maternal-fetal medicine or Level III/IV NICU care that a mother and baby need. PHI Air Medical closes that distance. Our flight crews deliver specialized high-risk pregnancy air transport care in the air, connecting rural patients to the right facility in time. And a PHI Cares membership protects your household from the cost of that flight — with $0 out-of-pocket for medically necessary transports on PHI Air Medical aircraft.
This guide walks you through the most common obstetric and neonatal emergencies that call for air medical transport, how PHI Air Medical flight crews respond, and why enrolling in PHI Cares membership before baby arrives is one of the smartest moves an expecting family can make.
Why Rural Mothers Need Air Medical Transport
Rural women face longer distances to specialized obstetric care than urban women, and that distance shapes outcomes. The Centers for Disease Control and Prevention (CDC) reports that roughly 80% of pregnancy-related deaths in the United States are preventable with timely, high-level care.1 Hemorrhage, severe preeclampsia and eclampsia, and infection are leading causes — and every one of them demands fast access to a hospital equipped for high-risk obstetrics.
When a rural hospital identifies a patient beyond its capability, the team calls for an interfacility air ambulance transfer to a maternal-fetal medicine center or a hospital with a Level III or Level IV NICU. The speed of that transfer — and the quality of care during the flight — directly affects how mother and baby recover.
PHI Air Medical serves exactly this gap. We operate more than 80 air medical bases across the United States, with flight crews trained to deliver advanced care from liftoff to landing. PHI Cares membership benefits apply across our 68 PHI Cares membership service area bases. You can check whether your area is covered on our coverage map.
Obstetric Emergencies That Call for Air Medical Transport
Not every pregnancy complication requires a helicopter. But several conditions escalate so fast — or occur so far from specialized care — that air medical transport is the only way to reach the right facility in time.
Severe Preeclampsia and Eclampsia
Preeclampsia — high blood pressure and organ dysfunction in pregnancy — affects roughly 1 in 20 pregnancies in the United States.2 When it worsens into severe preeclampsia or eclampsia, the risk of stroke, seizure, and organ failure climbs fast. PHI Air Medical crews start IV magnesium sulfate to prevent seizures, manage blood pressure medications, and monitor both mother and baby all the way to a maternal-fetal medicine center.
Placental Abruption
Placental abruption — when the placenta separates early from the uterine wall — can cause sudden maternal bleeding and cut off oxygen to the baby within minutes. PHI Air Medical carries warmed whole blood on board most aircraft, so our crews can begin hemorrhage control during the flight instead of waiting for arrival. Learn more in our blog, Blood on Board: How Blood Products in the Air Help Save Lives.
Premature Labor at Early Gestational Ages
A baby born at 24, 25, or 26 weeks needs a Level III or Level IV NICU the moment they arrive. When preterm labor begins at a hospital without that capability, the safest move is to transfer the mother — baby still on board — to a facility that can deliver the right care. PHI Air Medical crews manage preterm labor in the air, slow contractions when clinically appropriate, and keep continuous eyes on both patients throughout the flight.
HELLP Syndrome
HELLP syndrome is a severe variant of preeclampsia involving Hemolysis, Elevated Liver enzymes, and Low Platelets. It often appears without warning and calls for immediate delivery and intensive maternal care at a hospital equipped for high-risk obstetrics. Air medical transport bridges that gap.
Postpartum Hemorrhage
Postpartum hemorrhage — heavy bleeding after delivery — is a leading cause of maternal mortality worldwide.3 When a rural hospital cannot control bleeding with the tools on hand, air ambulance transport to a facility with advanced surgical and interventional resources becomes critical. PHI Air Medical crews can transfuse blood products during the flight, giving patients the best possible chance of a stable arrival.
Neonatal Emergencies: When a Newborn Needs Immediate Transport
Some air medical responses involve the newborn, not the mother. Babies with respiratory distress, congenital heart defects, neonatal sepsis, or hypoxic-ischemic encephalopathy need NICU-level care that their delivering hospital may not offer. PHI Air Medical crews trained in neonatal transport use isolettes, neonatal ventilators, and infant-appropriate IV access to stabilize and move these tiny patients safely from birth hospital to receiving NICU.
How PHI Air Medical Flight Crews Support High-Risk OB Patients
Every PHI Air Medical flight carries a critical care flight nurse and a flight paramedic. At bases that serve communities with frequent obstetric transfers, crew members maintain specific competencies in high-risk OB and neonatal care. Here’s what that means in practice:
- Continuous maternal and fetal monitoring during the flight
- IV magnesium sulfate and antihypertensive medication management
- Warmed whole blood transfusions on board for hemorrhage emergencies
- Emergency delivery management and neonatal resuscitation if needed
- Real-time communication with the receiving maternal-fetal medicine team
That last point matters more than most people realize. By the time the aircraft lands, the specialists at the receiving hospital are already briefed and ready. Care continues without a pause. For more on how air medical services bridge the rural healthcare gap, read our blog, The Essential Role of Air Ambulance Services in Rural Healthcare.
How PHI Cares Membership Protects Your Family — With $0 Out-of-Pocket
An air ambulance flight for a high-risk obstetric patient involves a specialized aircraft, a highly trained crew, advanced monitoring and medication, and often blood products — all on short notice. Even with solid health insurance, families can face deductibles, coinsurance, and out-of-network bills that add up fast.
A PHI Cares membership removes that worry completely. When a PHI Cares member takes a medically necessary flight on PHI Air Medical — including an obstetric or neonatal transfer — we bill the insurance company directly, accept what insurance pays as payment in full, and absorb the rest. The member household pays $0 out-of-pocket.
For a family already facing a high-risk pregnancy, that protection is a relief. The focus stays on mom and baby — not on what the flight will cost.
One Membership Covers Your Entire Household
A PHI Cares household membership covers every eligible member of the household under one affordable enrollment. A pregnant family member, a partner, children, and household dependents are all protected for medically necessary PHI Air Medical flights. Enroll once, protect everyone.
Enroll Before Baby Arrives
PHI Cares membership must be active before a flight occurs — it cannot be applied after the fact. If you’re expecting, especially in a rural area or with known risk factors, enroll well before the third trimester to make sure protection is in place when you need it most. Join PHI Cares today at phicares.com/memberships and give your family the peace of mind every expecting household deserves.
Frequently Asked Questions
What obstetric emergencies most commonly require air medical transport?
The most common obstetric emergencies requiring air medical transport are severe preeclampsia and eclampsia, placental abruption, premature labor at early gestational ages, HELLP syndrome, and postpartum hemorrhage — especially when these conditions occur at rural hospitals without the resources to manage them.
How does PHI Cares membership cover high-risk pregnancy air transports?
When a PHI Cares member takes a medically necessary flight on PHI Air Medical — including an obstetric or neonatal interfacility transfer — PHI Cares bills the insurance company directly, accepts the insurance payment as payment in full, and absorbs the rest. The member household pays $0 out-of-pocket.
Does PHI Cares membership cover my whole family, including a pregnant household member?
Yes. One PHI Cares household membership covers every eligible member of the household — a pregnant family member, a partner, children, and dependents — for medically necessary PHI Air Medical flights. Enroll once and protect everyone.
When should a pregnant person enroll in PHI Cares?
Enroll before an emergency occurs. For expecting families — especially in rural areas or with known risk factors — sign up well before the third trimester to make sure coverage is active if a high-risk complication arises.
Does PHI Air Medical transport newborns as well as mothers?
Yes. PHI Air Medical flight crews trained in neonatal transport care for newborns needing NICU-level care that isn’t available at the delivering hospital, including respiratory distress, congenital heart conditions, and neonatal sepsis.
Where does PHI Air Medical operate?
PHI Cares membership benefits apply across 68 PHI Cares service area bases. Check our coverage map at phicares.com/coverage-map to see if your area is covered.
Sources
1 Centers for Disease Control and Prevention (CDC). Pregnancy-Related Deaths. cdc.gov/maternal-mortality
2 American College of Obstetricians and Gynecologists (ACOG). Gestational Hypertension and Preeclampsia: ACOG Practice Bulletin. acog.org/clinical/clinical-guidance/practice-bulletin/articles/2020/06/gestational-hypertension-and-preeclampsia
3 World Health Organization (WHO). Maternal Mortality Fact Sheet. who.int/news-room/fact-sheets/detail/maternal-mortality